Blood Groups and Rh Factor is an important topic in Science and Technology that explains the classification of human blood based on antigens and the Rh factor present on red blood cells. Understanding blood groups is essential for safe blood transfusions, pregnancy care, and medical diagnosis. Under this topic, we will study the ABO blood group system, Rh factor, compatibility, and their medical significance.
Blood
Blood is a fluidic living tissue which is thick, sticky and red-coloured and flows into the blood vessels. This is made up of:
- Plasma (non-living liquid medium)
- Blood Corpuscles (living cells).
Plasma functions:
- Transports nutrients absorbed by the intestine to various body organs.
- Carries harmful substances from different organs to excretory organs.
Types of Blood Cells (Blood Corpuscles)
Three different types of Blood Corpuscles are found in the blood, all produced in the bone marrow via hematopoiesis, crucial for maintaining health:
- Red Blood Cells (RBCs / Erythrocytes):
- Function: Transport oxygen from lungs to tissues and carbon dioxide back to lungs.
- Key Feature: Contain hemoglobin, which binds oxygen and gives blood its red color.
- White Blood Cells (WBCs / Leukocytes):
- Function: Crucial part of the immune system, defending against infections and foreign invaders.
- Types:
- Neutrophils: Engulf and digest bacteria (phagocytosis).
- Lymphocytes: (T cells, B cells, NK cells) Involved in specific immune responses.
- Monocytes: Transform into macrophages (large phagocytic cells).
- Eosinophils: Combat parasitic infections and regulate allergic responses.
- Basophils: Release histamine in inflammation and allergic reactions.
- Platelets (Thrombocytes):
- Function: Essential for blood clotting and wound healing, preventing excessive bleeding.
- Nature: Small cell fragments, not complete cells.
Blood cell disorders, such as anemia (reduced red blood cells), leukemia (cancer of blood-forming tissues), and various immune deficiencies, can impact the health and well-being of an individual.
Types of Antibodies
- Antibodies are classified by five heavy polypeptide chains: α (Alpha), γ (Gamma), δ (Delta), ε (Epsilon), and μ (Mu), resulting in five antibody types.
- IgG is the main antibody in blood and body fluids, has the highest serum concentration, and is the only one to cross the placenta and reach to the embryo.
- IgM is the first antibody produced in response to an antigen; it has a pentameric structure.
- IgA has a dimeric structure and is the main antibody found in mother’s milk, vital for newborn immunity.
- IgE works on basophils and mast cells, participating in allergic reactions.
- IgD, IgE, and IgG are monomeric.
Types of Antibodies and Heavy Polypeptide Chains
| S.No. | Type of Antibody | Present Heavy Polypeptide Chain |
| 1. | IgG | γ (Gamma) |
| 2. | IgM | μ (Mu) |
| 3. | IgA | α (Alpha) |
| 4. | IgE | ε (Epsilon) |
| 5. | IgD | δ (Delta) |
Blood Groups
Firstly, Karl Landsteiner, an Austrian scientist, in 1901 classified blood into different blood groups.
What Determines Blood Groups?
- What decides the group is the presence or absence of antigens (A, B, Rh) on the surface of red blood cells (RBCs).
- Antigens are special proteins or sugars present on the surface of RBCs.
- Blood groups are mainly classified into ABO and Rh systems.
- The ABO system depends on A and B antigens.
- The Rh system depends on the Rh antigen (also called D antigen).
- Antibodies in plasma target absent antigens.
In the ABO blood group system:
- Type A: A antigen present. Has anti-B antibodies.
- Type B: B antigen present. Has anti-A antibodies.
- Type AB: Both A & B antigens. Has no anti-A or anti-B antibodies (universal recipient).
- Type O: RBCs do not contain A or B antigens. Therefore, recipient antibodies cannot attack these RBCs. Thus, Type O blood can donate RBCs to A, B, AB, and O groups (universal donor for red blood cells).
- Has both anti-A and anti-B antibodies. Therefore, Type O cannot receive blood from other groups except O.
| Blood Group | Antigens/Agglutinogens | Antibodies/Agglutinins |
| A | A | b (anti-B) |
| B | B | a (anti-A) |
| AB | A & B | Absent |
| O | Absent | a & b |
Rh Factor Basics:
- In addition to the A and B antigens, there is a protein called the Rh factor, which can be either present (+) or absent (–).
- Rh (Rhesus) factor is a protein of about 417 amino acids. It was discovered in a species of monkey named Rhesus macaques (Macaca mullatta).
- If the Rh antigen is present → blood group is positive (+) → Rh+.
- If absent → blood group is negative (–) → Rh-.
- About 85% of the human population in the world is Rh+, while the remaining 15% is Rh−.
- Rh Factors in Humans: Rh D (85%), Rh E, Rh e, Rh C, Rh c.
Blood Transfusion
- This is a method in which blood or blood products like platelets, plasma, etc. are transferred from the circulatory system of one person to another.
- Rules of Blood Transfusion
- During a blood transfusion, the donor’s blood must be compatible with the receiver’s blood.
- If mismatched blood is given, the receiver’s antibodies will attack the donor’s RBCs, causing them to clump together (agglutination) and burst (haemolysis), which can be fatal.
- Types of Blood Transfusion
- Allogenic Transfusion – Such a transfusion in which blood collected from other persons is used.
- Autogenic Transfusion – Such a transfusion in which blood collected from the person itself is used.
Some Important Points
- Rh− blood can be given to both Rh− and Rh+ patients.
- Rh− blood has no Rh protein, so:
- Safe for Rh− patients (no foreign protein).
- Safe for Rh+ patients (absence of Rh protein doesn’t cause reaction).
- Hence, Rh− = universal donor for Rh compatibility.
- Rh− blood has no Rh protein, so:
- Rh+ blood can be given to Rh+ patients only.
- Rh+ blood has the Rh protein.
- If given to Rh− patients, their immune system treats Rh protein as foreign → forms anti-Rh antibodies.
- Leads to Hemolytic Transfusion Reaction (HTR)→ dangerous.
- Therefore, Rh+ must not be transfused to Rh− patients..
Quick Table (Blood Transfusion)
| Donor →Patient↓ | O– | O+ | A– | A+ | B– | B+ | AB– | AB+ |
| O– | ✔ | ✗ | ✗ | ✗ | ✗ | ✗ | ✗ | ✗ |
| O+ | ✔ | ✔ | ✗ | ✗ | ✗ | ✗ | ✗ | ✗ |
| A– | ✔ | ✗ | ✔ | ✗ | ✗ | ✗ | ✗ | ✗ |
| A+ | ✔ | ✔ | ✔ | ✔ | ✗ | ✗ | ✗ | ✗ |
| B– | ✔ | ✗ | ✗ | ✗ | ✔ | ✗ | ✗ | ✗ |
| B+ | ✔ | ✔ | ✗ | ✗ | ✔ | ✔ | ✗ | ✗ |
| AB– | ✔ | ✗ | ✔ | ✗ | ✔ | ✗ | ✔ | ✗ |
| AB+ | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
Here: ✔ = Compatible | ✗ = Not compatible.
Universal Donor (Type O → O–)
- Our blood type is decided by the antigens (markers) present on red blood cells.
- Group O– blood does not have A antigen, B antigen, or Rh antigen.
- Because of this, when O– red blood cells are given to any person, the recipient’s body does not see them as “foreign” and does not attack them.
- So O– blood can be safely given to any patient regardless of their own blood group.
- That is why O– is called the universal donor for red blood cell transfusions.
Important note: O– blood plasma has anti-A and anti-B antibodies, but in transfusions we mainly focus on the antigens on red blood cells, not antibodies in plasma.
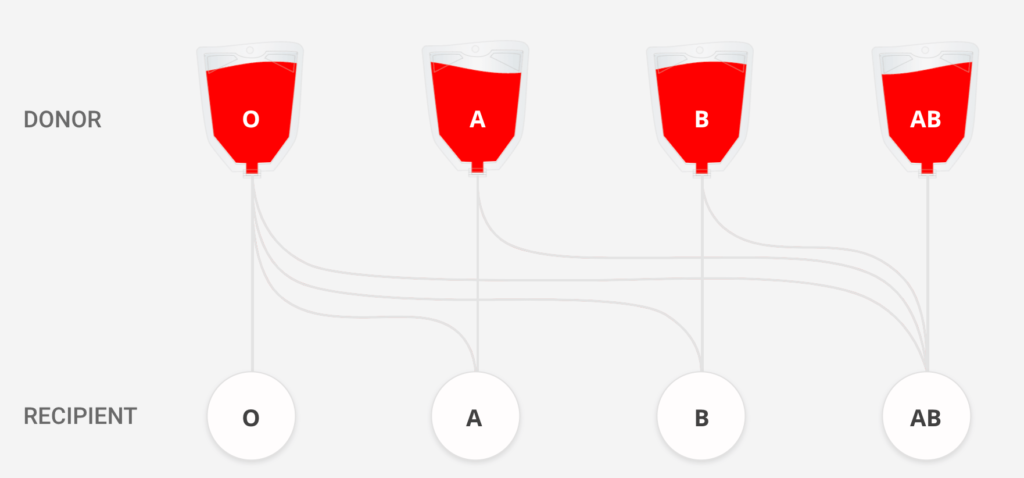
Universal Recipient (Type AB → AB+)
- Because Type AB blood has no antibodies in its plasma, it has no security guards to attack incoming blood.
- Therefore, a person with AB blood can safely receive blood from anyone.
Diseases or Infections Related to Blood Transfusion
- The following diseases or infections can occur due to the carelessness observed during the transfusion:
- HIV-1 and HIV-2 (Human Immuno deficiency Virus)
- HTLV 1 and HTLV-2 (Human T-Lymphotropic Virus)
- Hepatitis-B and Hepatitis C
- Creutzfeldt-Jacob disease etc.
Agglutination
- Agglutination is a reaction that occurs when particles, like bacteria or red blood cells, clump together in a liquid.
- It happens when an antigen, a molecule that can trigger an immune response, is mixed with its corresponding antibody at the right temperature and pH.
- The antibodies, called agglutinins, bind to the antigens and form a lattice-like structure.
- Antigen is called Agglutinogen.
| Blood Group | Antigens/Agglutinogens | Antibodies/Agglutinins |
| A | A | b |
| B | B | a |
| AB | A & B | Absent |
| O | Absent | a & b |
Blood Group Testing (Agglutination Test)
- Blood grouping is done by mixing blood cells with anti-A, anti-B and Anti-Rh sera (Anti-D sera), which contain antibodies against A, B and Rh (D) antigens respectively.
- Agglutination = clumping of red blood cells (RBCs).
- This occurs when antibodies in the test serum bind to their matching antigens on the RBC surface.
- Agglutination → corresponding antigen present.
- Agglutination
- with anti-A serum → A antigen present.
- with anti-B serum → B antigen present.
- with anti-Rh serum → Rh+.
- no agglutination → antigen is absent.
1. A blood sample is tested in the lab which shows the following reactions:
- Anti-A serum → Agglutination
- Anti-B serum → Agglutination
- Anti-Rh serum → No reaction
Which blood group is it?
- AB+
- AB–
- O–
- B–
- Question not attempted
Answer : ( 2 )
Explanation:
- Reaction with Anti-A → clumping → A antigen is present.
- Reaction with Anti-B → clumping → B antigen is present.
- No reaction with Anti-Rh → no Rh antigen → Rh negative.
- Thus, the blood group is AB–.
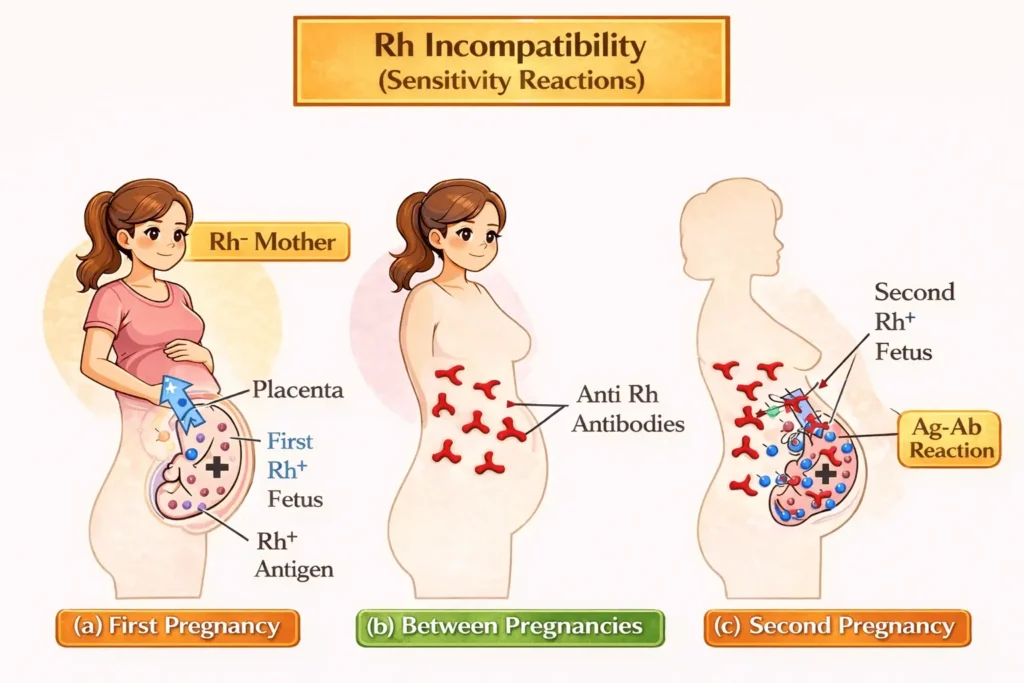
Rh incompatibility
What is Rh incompatibility?
- When a pregnant woman has Rh-negative blood and her baby has Rh-positive blood, there can be a problem called Rh incompatibility.
- This situation can happen because the baby inherits Rh-positive blood from the father.
- Rh incompatibility leads to Hemolytic Disease of the Newborn (HDN) (or Erythroblastosis Fetalis).
Why does it happen? (the reason)
- When the Rh-negative mother’s body comes in contact with Rh-positive blood cells from the baby (usually during delivery or any bleeding), her immune system thinks the Rh protein on the baby’s red blood cells is a foreign attacker.
- So, the mother’s body starts making antibodies against Rh-positive cells.
- The first baby is born unaffected (normal). Complications may arise during the second pregnancy.
- If in the second pregnancy the baby is also Rh-positive, these antibodies can cross the placenta and attack the baby’s red blood cells, causing serious problems.
- RhoGAM is administered to prevent this condition.
- Mother Rh– + Fetus Rh+ → fetal cells enter mother → mother forms anti-D → next Rh+ fetus → antibodies cross placenta → fetal RBC destruction.
RhoGAM (Rh Immunoglobulin)
- RhoGAM is a medication composed of Rho(D) immune globulin, which contains antibodies against the Rh antigen (IgG anti-D antibodies) found on red blood cells.
- Given to Rh negative pregnant women at risk of sensitization to Rh+ fetal RBCs.
- Mechanism of Action
- RhoGAM antibodies bind to Rh+ fetal RBCs in maternal blood.
- Mask & clear them → prevents maternal sensitization.
- Stops production of anti-Rh antibodies (alloimmunization prevention).
Blood Group Heredity
- Many different blood types are found in humans. They are addressed as ABO blood group system.
- ABO Blood Group System:
- Determined by three alleles: Iᴬ, Iᴮ, and Iᴼ or i (part of the same gene).
- Iᴬ produces Antigen A on Red Blood Corpuscles (RBCs).
- Iᴮ produces Antigen B on RBCs.
- Iᴼ (i) is recessive and does not produce any blood antigen.
- Inheritance and Expression:
- Blood group expression depends on the interaction of any two alleles.
- Six gene formats (genotypes) for blood are found in humans.
- Blood group O results from a homozygous recessive gene interaction (i i or Iᴼ Iᴼ).
- Follows Mendelian inheritance.
Genotype of Blood Groups
| S.No. | Blood Type | Genotype |
| 1. | A | Iᴬ Iᴬ, Iᴬ i |
| 2. | B | Iᴮ Iᴮ, Iᴮ i |
| 3. | AB | Iᴬ Iᴮ |
| 4. | O | i i |
Applications of Blood Group Inheritance
- To solve paternity disputes
- Blood transfusions
- Treatment of neonatal blood hemolysis and hereditary disorders like hemophilia etc.
Examples
1. A woman with blood group O+ is pregnant. The father of the child is AB–.
Explanation:
- Father (AB-) and Mother (O+): A child cannot inherit an O blood type from these parents because the father only provides A or B alleles, and the mother can only provide an O allele. Hence, it is impossible for their child to have blood type O (the child must inherit at least one A or B allele from the father).
Father: AB-, Mother: O+
| Mother →Father↓ | O | O |
| A | AO (Blood group A) | AO (Blood group A) |
| B | BO (Blood group B) | BO (Blood group B) |
2. A couple have blood groups AB+ and A–.
Explanation:
ABO blood group part
- Parent 1 (AB) has genotype IA IB — so their sperm/egg gives either IA or IB.
- Parent 2 (A) can be IA IA or IA i (A can be homozygous or a carrier of O). So they give IA or sometimes i.
Possible children
| Parent 1 → Parent 2↓ | IA | IB |
| IA | IA IA (Blood group A) | IA IB (Blood group AB) |
| i | IA i (Blood group A) | IB i (Blood group B) |
- So possible ABO types for the child: A, B, or AB.
- O is not possible because the child needs ii for O, but the AB parent has no i (O) allele to give.
Rh (positive/negative) part
- AB+ parent is Rh positive: genotype could be DD or Dd.
- A– parent is Rh negative: genotype dd.
- If AB+ parent is DD → all children will be Rh+.
- If AB+ parent is Dd → children can be Rh+ (Dd) or Rh– (dd).
- So both Rh+ and Rh– children are possible (Rh– possible only if the AB+ parent is heterozygous Dd).
3. A child has blood group AB. Determination of biological parents of the child.
Explanation:
Child’s blood group: AB
- AB child’s genotype = IA IB (must get A allele from one parent and B allele from the other).
- So, at least one parent must carry A (A or AB) and one must carry B (B or AB).
Now, Check each couple:
- A and B → A parent can give IA, B parent can give IB → AB possible.
- AB and O → AB (IA IB) can give IA or IB, but O (ii) can give only i → children are IA i (A) or IB i (B) → never AB.
- AB and A → AB can give IB, A can give IA → AB possible.
- B and AB → B can give IB, AB can give IA → AB possible.
Other Blood Group Systems
Bombay Blood Group (hh phenotype)
- Discovered in 1952 by Dr. Y. M. Bhende in Bombay (now Mumbai).
- Cause: Absence of H antigen on red blood cells.
- Characteristics:
- Neither A nor B antigens present.
- Anti-H antibodies present in plasma.
- Extremely rare (1 in 10,000 in India, rarer worldwide).
- Compatibility:
- Can donate to all ABO blood groups (A, B, AB, O) if Rh factor matches.
- Cannot receive blood from any ABO blood group (including O group → O has H antigen → anti-H reaction) due to anti-H antibodies.
- Can only safely receive blood from another Bombay blood group (hh) donor.
Cromer Blood Group System
Cromer Blood Group System
- One of 47 internationally recognized blood group systems.
- A blood group system based on antigens associated with glycoproteins in red blood cell membranes.
- Includes both common and rare antigens.
- Antibodies against rare antigens may develop due to: pregnancy, transfusion, or genetic mutations.
News: In 2025, scientists from India and the UK identified a new, extremely rare blood group called CRIB in a 38-year-old woman from Kolar, near Bengaluru, Karnataka.
What is the CRIB Blood Group?
- CRIB stands for Cromer India Bengaluru → Cromer (blood group system) and India-Bengaluru (the location of discovery).
- It is a new antigen under the Cromer (CR) blood group system.
- Classification: Not linked to ABO or Rh systems; it falls under the INRA (Indian Rare Antigen) system.
Uniqueness of CIRB:
- Absence of a high-prevalence antigen → causes panreactivity → blood was incompatible with all known donor samples → makes transfusion nearly impossible.
- Only one known individual with CRIB blood type globally → rarest blood group ever discovered.
Comparison of Rare Blood Groups: Bombay vs CRIB vs Rh-null
| Feature | Bombay Blood Group (hh) | CRIB Blood Group | Rh-null Blood Group |
| Discovery | 1952, Dr. Y.M. Bhende, Mumbai | 2025, Kolar (Karnataka, India) by Indian & UK scientists | 1961, Australia |
| System | ABO-related (absence of H antigen) | Cromer system (INRA – Indian Rare Antigen) | Rh system (absence of all Rh antigens) |
| Key Characteristic | Lacks H antigen (so cannot express A/B/O properly) | Absence of a high-prevalence Cromer antigen | Lacks all Rh antigens on RBC surface |
| Frequency | ~1 in 10,000 in India; rare globally | Only 1 known individual worldwide | Fewer than 50 known individuals worldwide |
| Compatibility | Can donate to anyone in ABO, but can only receive from another Bombay | No compatible donor identified so far (panreactivity with all known samples) | Universal donor for Rh-null patients, but can only receive from Rh-null |
| Medical Challenge | Transfusion crisis if not detected; often misdiagnosed as O group | Transfusion nearly impossible due to incompatibility with all samples | Extremely difficult transfusion; very rare donors |
| Importance | Highlights India’s genetic diversity in blood groups | Marks India’s contribution to discovery of new rare antigen | Known as “Golden Blood” → crucial for research & transfusion medicine |
| Relevance for India | Higher incidence in India (esp. Maharashtra, Gujarat) | First-ever global discovery from India (Karnataka, 2025) | Rare but medically critical, India may need to maintain registry |
